When creating a competitive benefits package, HR leaders usually look to their company’s specific offerings. That’s a strong strategy but it isn’t the only way to retain your people and attract new talent.
You should also consider the actual structure of your benefits plan – specifically, whether a cafeteria plan that allows for pre-tax salary deductions for health and other benefits is beneficial for your employees and organization. While cafeteria plans can incorporate several benefit components, they can also be as simple as a premium only plan (POP).
What is a Premium Only Plan?
A premium only plan (POP) falls within the Internal Revenue Code’s Section 125, which lets employees use some of their earnings before taxes to pay for group insurance and other pre-tax contributions. It’s the simplest form of a cafeteria plan and a smart way for employers and employees to save on taxes.
Beyond the umbrella term of health insurance premiums, POPs can encompass various insurance products (including group term life insurance, disability insurance, and even dietary supplements), provided they align with the cafeteria plan’s rules.
Why You Should Offer a 125 Plan
Imagine your ideal benefits plan. Does it involve saving everyone money, empowering employees to be their best selves, or elevating your company’s competitive edge?
If you answered any (or all), you’re in luck. A POP is a win-win scenario where employees gain access to a cafeteria plan without bearing the full brunt of associated costs, and employers amplify their benefits offerings.
Moreover, integrating a 125 cafeteria plan nurtures your workforce and signals that you’re committed to fostering a supportive and financially savvy work environment. Offering a POP allows you to:
- Save everyone on pre-tax deductions: Employers realize 7.65% in FICA tax savings, and employees average 25% tax savings.
- Invest in your team’s financial well-being.
- Set the stage for attracting the 80% of candidates who believe financial wellness is an integral part of a comprehensive benefits package.
- Provide a menu of benefits that employees can tailor to their unique needs, enhancing their satisfaction and loyalty.
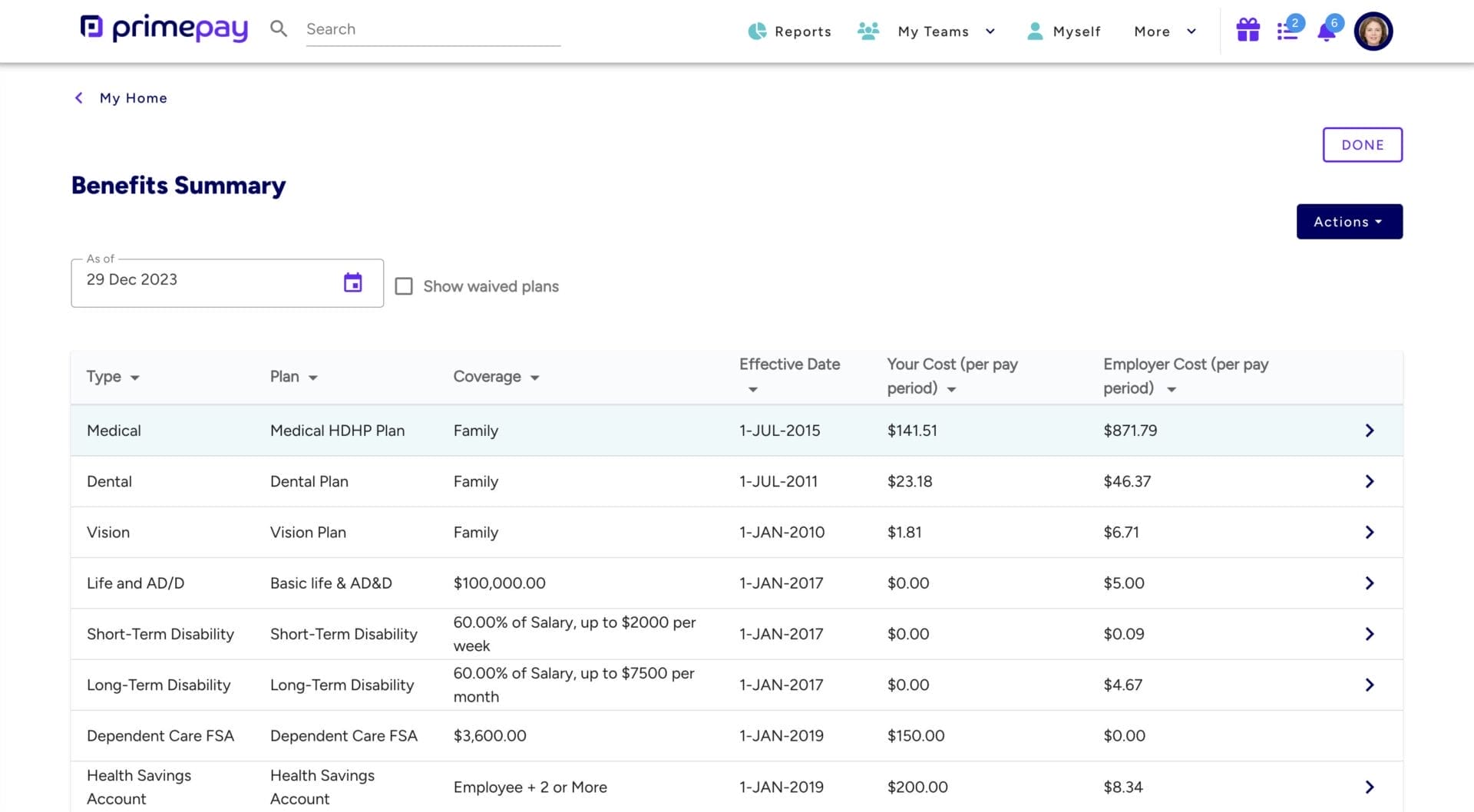
Allowing employees to select benefits on their own time and for their unique needs adds value to the employee experience and ensures people will choose the plans and pre-tax savings that are right for them.
Maximizing Tax Savings with Cafeteria Plans
A 125 plan should be a part of your strategic financial planning, as it offers businesses and their employees a wealth of potential tax savings (pun intended). By skillfully navigating payroll taxes, a POP plan strengthens the financial defenses of both parties against unnecessary tax liabilities.
Whether it’s a health savings account, a flexible spending account, or even Archer medical savings accounts, pre-tax contributions made to these vehicles under a Cafeteria Plan can significantly reduce the tax burden.
Employer Benefits: Reducing Overhead with POP
The POP plan is a practical approach to managing overhead costs for employers. By embracing this plan, you can effectively shrink your taxable payroll. The result? Substantial savings, especially for many employers within the professional services sector.
For example, let’s say small company Jerry’s Jungle Gyms offers a premium only plan. A possible scenario may look like the following:
- Each of the 20 employees chooses to contribute $3,000 pre-tax to their group health insurance through the POP.
- The collective reduction in taxable income can lead to an estimated annual tax windfall of $4,590, which provides a tangible impact of nontaxable benefits on Jerry’s company balance sheet.
- Thus, Jerry’s offering of POP becomes a gesture of goodwill and a strategic move to retain talent and reduce costs.
How Employees Save Money with POP
Employees also find themselves in a favorable financial position using pre-tax dollars to pay for qualified medical expenses. By reducing their income taxes through pre-tax deductions, they witness a welcome boost in their take-home pay – a direct result of their lowered tax liabilities.
Consider employee Susan, who earns an annual salary of $60,000. By participating in the POP and reducing her taxable income to $57,000, Susan could see her take-home pay rise by approximately $1,725. This example illustrates the tangible benefits of the premium-only plan, where saving money isn’t just a catchphrase but an actual outcome of strategic financial planning.
Tip: Focus on employees’ financial literacy. Because over 60% of people say improving financial literacy is their top educational priority, you’ll empower your employees to use your benefit offerings confidently and signal to top talent that you’re invested in their future.
Avoiding Common Pitfalls of POP Implementation
While the benefits of a POP are clear, it’s essential to note potential drawbacks.
Employers must be vigilant in complying with the intricacies of Section 125 plans, ensuring that their POP plan is secured by formal written documentation and adheres to the stringent nondiscrimination rules.
The ‘use-it-or-lose-it’ rule is another aspect that demands attention, particularly with Flexible Spending Accounts (FSAs), a feature that employers can implement in their Cafeteria Plan. Employers must convey the importance of this rule to employees effectively and the constraints on altering Cafeteria Plan elections mid-year, which are only permissible during qualifying life events.
Tip: HR must use clear and repeated communication regarding benefits and financial resources. PWC found that only 68% of employees report using the financial wellness services their employer provides, indicating that most benefit reminders only happen during administration season instead of throughout the year.
The Role of a Third-Party Administrator in Managing a Cafeteria Plan
We’re not going to lie: Navigating benefits and employee questions can be time-consuming and confusing, which is why the expertise of a third-party administrator is invaluable. Many third-party administrators guide employers and help them:
- Create plan documents that comply with nondiscrimination rules and other regulations.
- Communicate the intricacies of the Cafeteria Plan to their employees.
- Educate participants on maximizing benefits.
- Conduct regular compliance reviews to ensure the plan remains up-to-date with any changes in legislation or IRS guidelines.
Furthermore, some third-party administrators and/or benefits advisors can offer valuable insights into optimizing the plan’s structure to better align with your company’s overall benefits strategy. They can recommend adjustments that enhance the plan’s effectiveness and employee satisfaction by analyzing participation data and employee feedback. This continuous improvement cycle ensures that the POP remains a valuable asset in your company’s benefits portfolio.
Eligibility and Participation Rules for POP
While companies of various structures – from S corporations to non-profits – can sponsor a Cafeteria Plan, not all individuals within these entities are eligible to reap the benefits. For instance, owners, shareholders, and their families may find themselves on the outside looking in when it comes to participation.
S corporation shareholders with over a 2% stake encounter unique restrictions under a Cafeteria Plan These individuals and their immediate family members are barred from participating—a rule extending to the intricate web of relationships, including spouses, children, and grandparents. This limitation underscores the need for S corporations to carefully consider the implications of their ownership structure on their ability to participate in a Cafeteria Plan.
Keep an eye on these eligibility nuances to maintain a fair and compliant plan with IRS regulations.
Maximize Pre-Tax Savings with a Cafeteria Plan
It’s clear that Cafeteria Plans offer a compelling blend of tax savings, employee satisfaction, and compliance considerations. Whether you’re an HR leader looking for new ways to retain top talent or a business owner weighing the benefits of implementing a Cafeteria Plan, the takeaway is undeniable: they help build a thriving, financially healthy work environment for everyone involved.